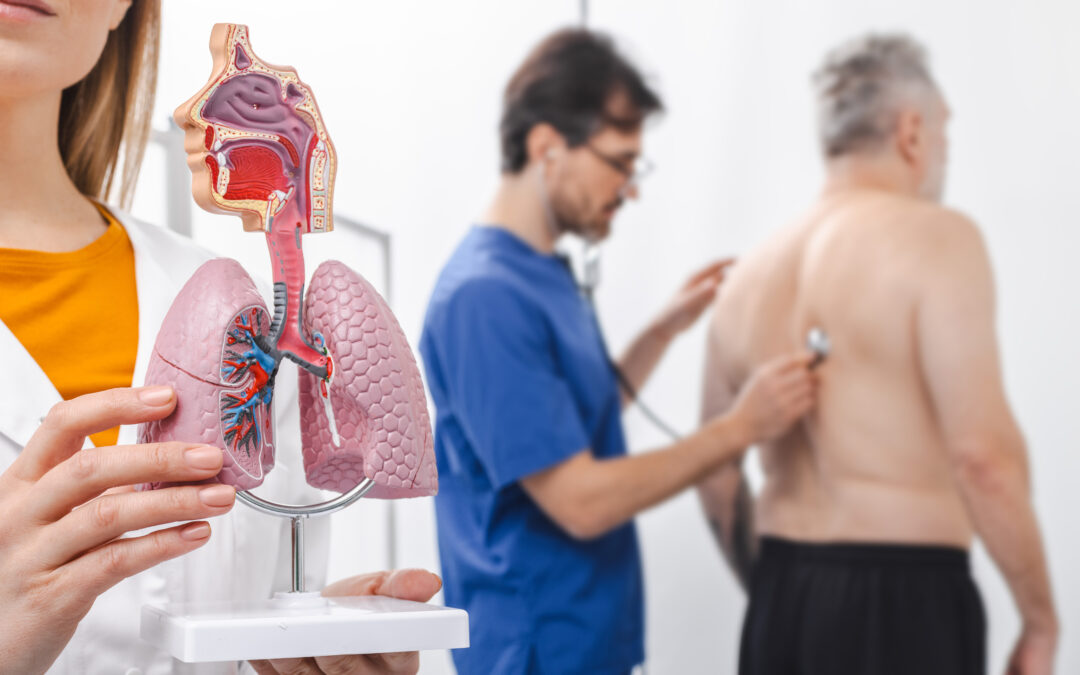
Why do we cough? Cough is a defense mechanism to clear irritants from our lungs. The process begins with a trigger like cold air, smoke, or aspirated food/liquid that then causes the body to respond by closing the glottis, thereby increasing intrathoracic pressure. Breath is then expelled at a high velocity, clearing out any foreign particles in the lungs. Occasional cough is therefore normal; a persistent cough on the other hand can be a sign of a medical condition.
Did you know that cough is one of the most common reasons people see a doctor every year? It is categorized by duration:
Acute: present < 3 weeks
Subacute: present 3 – 8 weeks
Chronic: present > 8 weeks
The most common cause for an acute cough in adults is a viral upper respiratory infection, i.e., the common cold. Other causes include rhinosinusitis, COPD exacerbation, rhinitis, asthma, pneumonia, gastroesophageal reflux (GERD) or CHF. These are conditions where cough is a symptom that can be treated and relieved. There is no consensus on the definition for chronic cough, but it has become clear that cough can be more than a symptom of an underlying disease for some patients; it is a medical condition in and of itself that can have significant impact on quality of life.
Unexplained chronic cough (UCC) is a cough that persists and is of unknown origin. UCC may also be identified as refractory chronic cough or difficult-to-treat cough. Globally, chronic cough is seen in 2-18% of the adult population, predominantly in middle age, with women reporting a higher incidence. Until puberty, the incidence is similar between boys and girls. However, children are not miniature adults and identifying and managing chronic cough in these patients is approached and handled differently.
The burden of UCC on patients can be significant and disabling for some, reducing quality of life and even leading to social isolation and depression. People experiencing UCC report fatigue, disrupted sleep, and in extreme cases, chest pain, rib fractures, and hernias. It can also exacerbate conditions such as incontinence. Patients may live with UCC for years before receiving effective treatment.
A thorough assessment that includes objective testing is important before a diagnosis of UCC can be made. Medical history, physical exam, and tests like spirometry or chest x-ray can be part of a full work-up to identify a potential disease state. Other tools to assess cough include cough diaries, cough counting measures, and quality of life questionnaires like the Leicester Cough Questionnaire. Asthma is a common cause of cough and needs to be ruled out. This could involve bronchial challenge testing with methacholine or mannitol to assess airway hyperresponsiveness as well as measurement of other markers of inflammation like FeNO (fractional exhaled nitic oxide) and blood or sputum eosinophils.
Identifying the cause of a patient’s cough will help identify the most effective treatment for that patient. There is growing recognition that there are endotypes and phenotypes for chronic cough and these play a role in treatment success. Recognized phenotypes of chronic cough include:
- Asthma – this common condition has three identified cough sub-groups: classic asthma, cough variant asthma and non-asthmatic eosinophilic bronchitis.
- Reflux cough – may entail recurring aspiration of gastric contents leading to airway inflammation.
- Postnasal drip syndrome – identified as upper airways cough syndrome (UARS) but there appears to be some controversy about this syndrome and why it causes cough.
- Iatrogenic cough – seen in approximately 15% of patients taking ACE inhibitors. Other drugs like calcium channel agonists may worsen already existing reflux disease, increasing cough.
- Smoking – there is a cumulative effect of on-going smoking, or exposure to, and chronic cough. Pack years (packs smoked per day X number of years) along with current consumption are predictors of cough frequency.
Treatment of UCC remains challenging and there are guidelines and recommendations from various groups. Unfortunately, many of the current pharmacological treatments are off-label and it is difficult to determine which will be best for each patient and which will yield the least adverse effects. In general, it is recommended that treatments be given in short trials and discontinued if there is no response. If it is shown that cough is diminished, a longer trial of several months may be indicated to see if the cough resolves. Non-pharmacological treatment of UCC includes cough control therapy and physical/speech therapy. A benefit of non-pharmacological treatment is that there are no adverse effects.
While cough is not a new problem, awareness of the burden of chronic cough is increasing along with the prevalence. This is an exciting area of research and development. With continued dedication, many people who have been affected by UCC may soon find relief.