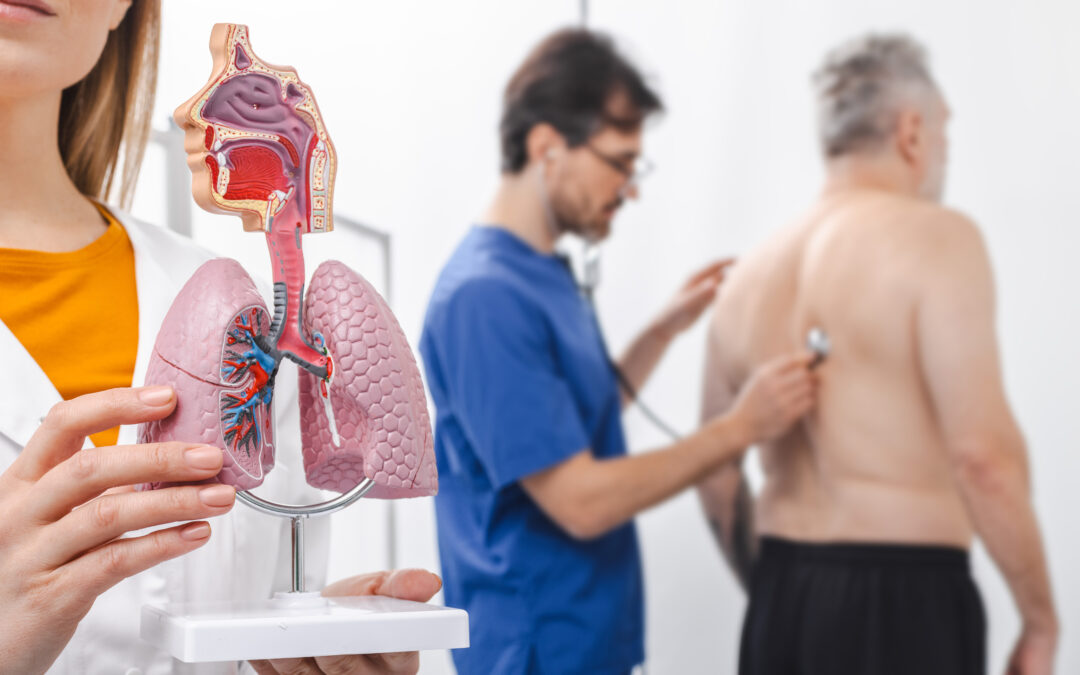
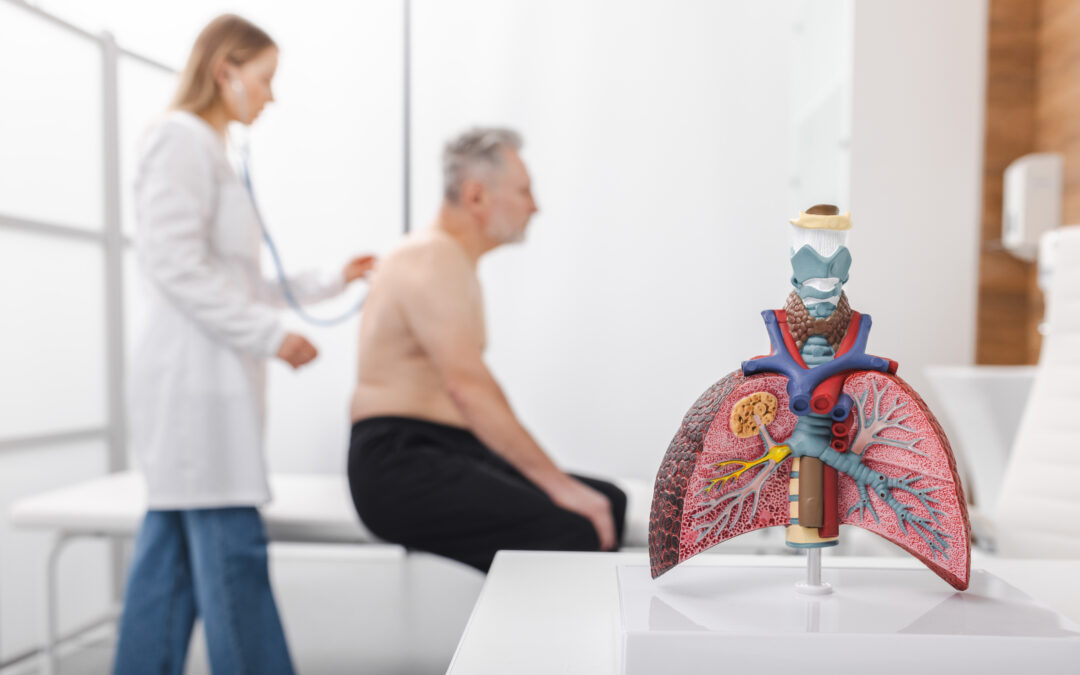
Your Brain and Breath— Airway Anatomy, Part 3

For the past two months, this blog has opened with: “How often do you think about breathing? Probably not too often—unless you find yourself struggling to breathe. Then breathing is all you can focus on.” Our breathing pattern is shaped by many factors, including activity level, emotions, and voluntary effort. Most of the time, breathing happens automatically, coordinated by the medulla (at the base of the brainstem) and the pons just above it. The cerebral cortex also gives us voluntary control—for example, taking a deep breath to blow up a balloon. Spinal circuitry helps organize the breathing muscles by integrating input from the brainstem. This is a simplified description of respiration as there is an integrated network of brain regions which can control and effect respiration.
Eupnea is quiet, rhythmic breathing at rest and is largely passive. Hyperpnea occurs when the body’s metabolic demands increase (for example, during exercise); at that point breathing becomes more active, with additional muscles and brain circuits recruited to move air in and out. One key function of breathing is ventilation—the movement of air into and out of the lungs—to bring oxygen in and remove carbon dioxide. Keeping blood gases in balance (oxygen, carbon dioxide, and pH) requires constant monitoring. Receptors in the airways and lungs provide continuous feedback about the body’s internal environment and can also trigger protective responses to irritants, inflammation, or other adverse exposures.
Key factors in this complex system.
Chemoreceptors in the carotid bodies (located in the neck) detect changes in oxygen (O2), carbon dioxide (CO2), and blood pH. When these variables drift from their ideal range, the carotid bodies signal for adjustments—often increasing respiratory rate and also influencing heart rate and blood pressure—in an effort to restore homeostasis.
Central chemoreceptors work with peripheral chemoreceptors in the carotid bodies to regulate arterial carbon dioxide (PaCO₂) and keep pH within a narrow range. Although multiple brain regions modulate breathing, the core chemosensitive and rhythm-generating circuitry is centered in the brainstem.
- Retrotrapezoid nucleus (RTN): Often described as a key site for central CO2/pH sensing and a major driver of ventilatory responses.
- Nucleus of the solitary tract (NTS): Integrates sensory input (including from peripheral chemoreceptors) and helps adjust breathing and other autonomic functions.
- Locus coeruleus: Shows increased activity in response to elevated CO2 (hypercapnia) and may be especially relevant during sleep, when stable ventilation is essential.
- Raphe nuclei: A group of nuclei spanning the midbrain, pons, and medulla that contribute serotonergic input to respiratory control and are also involved in sleep-wake regulation.
The vagus nerve (the 10th cranial nerve) is a major pathway of the parasympathetic nervous system (PNS)—often described as the “rest and digest” system. It supports involuntary functions such as digestion, heart rate, and aspects of breathing. The vagus nerve links the brainstem with organs in the chest and abdomen, including connections that influence the throat, heart, and lungs. In contrast, the sympathetic nervous system (SNS), coordinated in part through the hypothalamus, supports the “fight-or-flight” response. SNS activation can affect ventilation and contribute to faster, shallower breathing or hyperventilation. This pattern is commonly associated with stress, anxiety, and panic, but it can also be neurologic in nature.
Respiration and hormones.
Hormones also influence breathing. Thyroid hormones, for example, play an important role in respiratory development, and significant thyroid dysfunction can contribute to respiratory problems. Sex hormones can affect respiratory parameters as well; the presence and balance of progesterone, estradiol, and testosterone may help explain differences in breathing patterns between males and females and across the lifespan. In addition, increases in adipose tissue raise levels of leptin. In obesity, leptin signaling can become less effective (leptin resistance), which may contribute to conditions such as obesity hypoventilation syndrome and some forms of sleep-disordered breathing, including central sleep apnea.
This provides a high-level view of the brain and the respiratory system. This complex relationship constantly hums under the surface of our consciousness. When we zoom out, one theme becomes clear: breathing isn’t “just lungs.” It is essential to recognize the connections between various organs and systems in our body. Cardiorespiratory function must be effective to maintain health and vibrancy. Take good care of your lungs, heart and brain and they will take good care of you!
Author:
Heather Murgatroyd, BA, RRT, CPFT, AE-C
Senior Clinical Specialist
Methapharm Respiratory
References
- Nattie, A. Li. Central chemoreceptors: locations and functions. Compr Physiol. 2012;2(1):221–254.
- Krohn, M. Novello, R.S. van der Giessen, C.I. De Zeeuw, J.J.M. Pel, L.W.J. Bosman. The integrated brain network that controls respiration. eLife. 2023;12:e83654.
Brain Control of Respiration: Exploring the Neural Mechanisms Behind Breathing
https://neurolaunch.com/what-part-of-brain-controls-respiration/